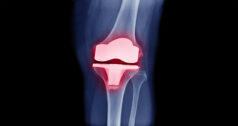
The use of additive manufacturing in orthopaedic implants continues to grow as OEMs seek to produce better products, more efficiently. The medical industry as a whole makes up one of the larger market shares of additive manufacturing, and it’s expected to increase along with additive manufacturing in the coming years. An October 2012 report from MarketsandMarkets stated, additive manufacturing will grow at CAGR of 13.5% from to 2012 to 2017 to reach $3.5 billion in 2017.
The State and Future of Additive Manufacturing in Orthopaedics, a panel discussion, is slated for the lineup at OMTEC 2013 in June. The three panelists started the conversation early, weighing in on the benefits and uses of the process.
Participants
- Andy Christensen, President and Owner, Medical Modeling Inc.
- Magnus René, Chief Executive Officer, Arcam AB
- Stephen Rouse, D.D.S., consultant and chairman of the Society of Manufacturing Engineers RTAM Medical Tech Group
What are the best ways in which to use additive manufacturing for orthopaedic devices? What are the benefits of using this process?
Andy Christensen: Additive manufacturing or AM finds its best application in producing products that are either highly complex, highly customized or where the quantity needed is small and other production techniques are not cost-effective. From a practical standpoint, today’s uses of additive manufacturing in the orthopaedic industry are mostly contained in three main application areas: 1) instrument and implant prototypes (plastic or metal), 2) patient-specific surgical guides/instruments and 3) manufacturing of porous or porous/solid implant constructs.
Prototypes are a “legacy” use of the technology that will continue to grow and do provide value; I think everyone reading this probably has an idea of this application. The production of patient-specific surgical guides and instruments has experienced heavy growth over the last five years with now all main players in total knee arthroplasty (TKA) space providing a system, using AM, for physical guidance (i.e.: with tactile, additively manufactured drilling and cutting guides) of placement of off-the-shelf TKA components. Several very public statements by OEM CEOs have led me to believe that this technology will impact not just three to four percent of the cases, but perhaps 50 percent of the cases performed, at some point. Very interesting opportunities still exist in this space as the technology begins to be applied outside of the TKA procedure.
The most exciting area in AM within orthopaedics for the near future, in my opinion, is with AM of implants. AM has the unique ability to provide “complexity for free,” and the application here is for unique, interesting porous surfaces or volumes. Imagine being able to design your own porous structure, integrating your specific “look,” dialing in pore size, interconnectedness, porous/solid volume, etc. and coming up with something unique. Great, now take that unique porous structure and apply it across your product line, and without secondary machining or manufacturing processes to adhere it to your parts as with some traditional techniques. Now you’ve got a uniform porous structure that can be applied at will to your product line, and the best part is that it’s not a surface; the surface is integral to the part as it is produced as a single, unified body during the construction of the implant via AM. These techniques are used both in Europe and the U.S. today for construction of implants that have been through the appropriate regulatory hurdles, including the FDA 510(k) clearance process.
Magnus René: The best opportunity is for sure to use AM to manufacture advanced trabecular structures.
Stephen Rouse: The greatest benefit to using AM lies in being able to create geometric designs that we’re unable to do with other existing technologies. A good example of that are the hip cups that had the welded beads on them. Those beads came off, and there’s a big lawsuit as a result of that. Being able to integrate that feature into the build for ingrowth of bone makes a phenomenal difference, and really can only be done adequately using this type of technology.
Along with that, the ability to do custom devices for a one-off type manufacturer is something that you can’t do with any of the traditional methods. The biggest part is the design itself—whatever happens to work best for the patients, rather than what is manufacturable.
Can OEMs change easily their processes to incorporate additive manufacturing?
Christensen: I’m going to focus my answer on use of AM for implant constructs in implantable metals. A major “plus” for at least the Electron Beam Melting (EBM) AM technique is that it is able to process and certify materials to the same ASTM and ISO standards for titanium alloy that are in current use. OEMs have material specifications that have been around internally for years, and have been substantiated through testing, validations, regulatory submissions, etc. If we can hold to the key elements of those specifications (strength, chemistry, microstructure, etc.) while enhancing them to be flexible for AM, we get a strong argument for the fact that AM isn’t a radical, new technique producing unknown materials. It’s just a different technique for processing the exact same materials in a different way.
As an aside, this question would imply that AM’s biggest opportunity exists to replace legacy manufacturing techniques of existing products. I don’t believe this is the case. AM will be able to offset machining or casting of certain components, sure. I’ve seen my share of proposals in which AM would reduce a part’s cost, compared to traditional manufacturing techniques, by 90 percent, and others where it’s not cost advantageous at all. But AM’s true value proposition lies in the fact that it can produce parts that no other manufacturing technique can produce. These include novel porous structures and constructs that open up new markets and new opportunities for the sale of devices that truly didn’t exist before AM. This is the value that AM brings to orthopaedic implant manufacturing.
René: Additive Manufacturing can help reduce lead time and tooling costs.
Rouse: I don’t think it’s a difficult thing to do, but I think what has to be kept in mind is that AM is not going to replace—at any time—the traditional manufacturing method. There is always going to be a place for the way OEMs are doing things now. The success will lie in using the technology that is most effective for the procedure they want to perform. For those devices that work best using traditional methods, continue to use the method you’re using, but the most bang for your buck is going to come from doing those things that you haven’t been able to do.
For instance, look at some of the hip cup designs coming out in Europe, with an integrated mesh ingrown area. That is something that we couldn’t do before, and AM makes the process much more feasible.
What limitations might OEMs face with additive manufacturing?
Christensen: Speaking about most AM processes, both plastics and metals, there is a learning curve with adopting the technology. Other manufacturing processes such as injection molding, CNC machining and investment casting have been around a long time and are very well-established. This means that the know-how for designing parts that will be successfully produced using these techniques exists, as does the know-how to actually use the technologies to successfully produce the parts. For AM this know-how exists, but in pockets of knowledge that may or may not be inside of the OEM. Putting it all together either requires a bit of time or help from an experienced AM partner. As an example, when using investment casting, the location of gates or sprues is critical to ensuring a good, consistent cast without voids. In AM, the equivalent know-how would be surrounding orientation of parts in the build chamber and use/placement of support structures. Depending on the part and the AM process, both orientation and supporting can impact several things, including surface finish, throughput, length of build, strength, etc. Certain porous structures in certain AM manufacturing methods also require more thoughtful consideration for orientation and supporting to be repeatable. These issues may or may not be “limitations,” but are areas in which OEMs could perceive a limitation based on lack of experience with these new technologies.
René: And, new production methods bring new products that have to be validated.
Rouse: The biggest limitation is going to be in the mindset of the education of the individual involved in the process. The engineers who do all of the designing, their whole thought process is wrapped around the traditional way of manufacturing. They must break out of that mold to understand that you design what’s most effective; you don’t design to manufacture anymore. When we work with surgeons and we’re doing custom devices, sometimes that’s difficult for them to even understand. You have to open your mind up, and we’ll show you a new way.
What developments are underway to enhance additive manufacturing?
Christensen: All of the technologies continue to advance and, as you can see by the stock market, AM is currently a very hot topic to investors. That given, we will continue to see new machines and new processes enter the market over the coming years. Primary focus for the “industrial” type AM machines will likely be toward expansion of material choices and better speed, which to me means more throughput. If we again focus on the application area of making implants, the speed enhancements will open up new markets. For example, today there is a potential product which needs to be made for $50 to be profitable. Much of the cost of the AM technologies is built into the capital cost of the machinery and the “system” needed for it to operate. Today, by AM, if you can make 50 of those parts in 24 hours, they cost you $100 to make. If the AM machine is then able to produce 100 of those parts in the same 24 hours, your cost will shrink, and for this example let’s say it shrinks to the magic level of $50 per part. This enhancement of speed has meant that an application area which was completely off-limits to AM because it was 2x too expensive now becomes feasible. Think of computers, a 2x increase in speed over some short period of time is reasonable, and it’s likely close to the same here—we will see those kinds of speed improvements over the course of several years, and it will have the impact of opening up completely new markets for AM.
René: Expect to see higher productivity systems that are adapted for easier validation.
Rouse: Materials. Again, much the same way manufacturing is based around materials that are available, some of the materials that we would like to use, we have not found a way of using effectively yet. There is going to be a lot of ability to move into the area of biologically-active materials which are going to be a tremendous benefit in this whole process. Instead of always having a foreign body to do a repair, for instance, when the materials are available, we’ll be able to insert a biologically-active femoral pin that has the necessary strength to do the job of supporting the fracture and, in the long run, will actually become a part of the bone itself and will not require removal or replacement in the future.
What haven’t we asked that would be beneficial for OEMs to understand about additive manufacturing?
Christensen: A last question might be whether the application of AM technology for implant production is far off, or is it really here today, for manufacturing not just prototypes, but implants. The answer is yes; many OEMs are either already using or are heavily investing in the future of the technology as a way to stay competitive, release novel products, reduce cost or a winning combination of all three. AM is set to play a major role in the manufacturing of tomorrow’s novel orthopaedic devices based on its flexibility, economies of scale for short runs and ability to produce parts of almost unlimited complexity.
René: It is important to understand that AM is a production method and that it is well suited for volume manufacturing. Today some 30,000 acetabular cups are manufactured yearly by companies using our EBM systems alone.
Rouse: We were given this earth to be good stewards of it, so conservation is an important part of the way we should deal with life. I don’t think we’re going to burn the planet down if we’re not careful about our manufacturing processes, but at the same time, if I can use 90 percent less material in doing a process, and if most of what I have shipped in to me is used in the process instead of turning into waste, then I have made much more effective the mining operations, the shipping operations, the use of fossil fuel to move things from one point to another, and my whole process becomes more cost- and environmentally-friendly.