Conventionally, PEEK, titanium-coated PEEK and titanium have been used as standard biomaterials for implants such as spinal interbody cages, but recent studies have shown shortcomings with these materials. A 2019 report published by FDA (Biological Responses to Metal Implants, September 2019) makes it evident that the Agency is no longer grandfathering classic alloys for use in medical devices and that events such as this FDA scrutiny will continue to drive the development and adoption of newer, more innovative materials.
Polymer Material Considerations
The ideal orthopedic material, particularly in spine, delivers necessary mechanical integrity, radiographic visibility, osseointegration and antibacterial performance.
In looking at the traditional materials:
- PEEK shows an elastic modulus comparable to that of cortical bone, but literature has illustrated that it consistently prompts a fibrotic and inflammatory tissue response, preventing it from integrating with host tissue.
- Titanium exhibits stronger osseointegrative properties when compared to PEEK, but it is radiopaque, which makes bone fusion assessments difficult as the bone/implant interface is often obscured in post-operative imaging. Furthermore, titanium implants carry a risk of stress shielding and tissue resorption as the metal material is much stiffer than surrounding bone in orthopedic applications. This can lead to implant failure and result in the need for revision surgery. In addition, corrosion and metallosis – as cited in the recent FDA report – are issues coming to the forefront.
- Recent workarounds include coating PEEK with titanium, resulting in similar drawbacks while adding the risks of delamination of the titanium coating, subsidence and the generation of wear debris.
OXPEKK® polymer – a formulation of polyetherketoneketone (PEKK) proprietary to Oxford Performance Materials, Inc. (OPM) – is 3D-printed via the OsteoFab® process to produce OsteoFab PEKK, a practical and beneficial material solution that provides all desirable device properties in a single product. In addition to its mechanical integrity and radiographic visibility, OsteoFab PEKK demonstrates inherent antibacterial characteristics as well as osseointegrative properties that were confirmed in a study that examined the in vivo material characteristics of PEEK, titanium-coated PEEK and OsteoFab PEKK in a sheep model.
Additive Manufacturing Leads to Optimized Surface
OsteoFab finished devices are manufactured from OXPEKK® IG100 powder via a laser sintering process that is also proprietary to OPM. Only laser light and IG100 powder are involved in the process; no additives, solvents or other materials are used. Purified compressed air is passed through a nitrogen generator that extracts and uses it to blanket the build chamber during the lasing process. The laser sintering machine (EOS EOSINT P 800) uses STL files to build the parts.
An important factor resulting from the additive manufacturing process is the inherent rough surface topography of OsteoFab devices. OsteoFab PEKK has an average surface roughness (Rq) of 26 μm (1022 μ in.) that creates a peak-and-pit surface topography that is much rougher in comparison to conventional PEEK material. Figure 1, below, illustrates this difference in surface roughness via Confocal Laser Scanning Microscopy (CLSM).


Figure 1: CLSM images of machined PEEK (left) and OsteoFab PEKK (right), which depict the rougher surface topography of PEKK.
Due to the material chemistry and surface energy of PEKK, when OsteoFab parts are laser sintered, successive layers bond strongly to one another to create dense, fully formed shapes. The rough surface topography of OsteoFab PEKK devices helps enable a number of performance benefits – namely osseointegration, antibacterial properties and a fluid wicking capability of the part surface. These functional advantages, driven by the right combination of material chemistry and manufacturing process, deliver more tailored solutions to meet today’s growing clinical needs.
What Have the Studies Shown?
Numerous studies on material and implant structure have detailed the benefits of OsteoFab PEKK for orthopedic applications.
Early in vitro studies (circa 2010) indicated a positive cellular response to OsteoFab PEKK and subsequent in vivo studies that examined tissue response to OsteoFab PEKK implants in an osseous environment (rabbit model, circa 2013) showed that native PEKK material supported bone apposition. OsteoFab PEKK showed no observable immunological rejection and no increase in inflammatory response cells. Figure 2, below, shows the in vivo bone response to OsteoFab PEKK compared to machined PEEK.
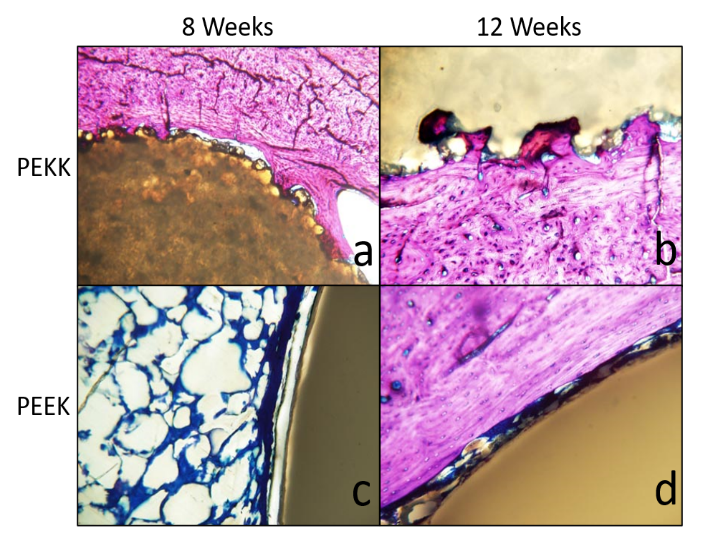

Figure 2: In vivo bone response to OsteoFab PEKK versus machined PEEK in a rabbit femoral model at 8 and 12 weeks. (a,b) Bone (pink) growing onto the surface of a PEKK rod implant and into the peaks and pits of the rough surface. (c) Fibrous tissue (blue) surrounding a PEEK rod implant. (d) Fibrous tissue (blue) present in the interface of a PEEK rod implant and existing femoral bone.
Shifting from studying the implant material response to implant structure and morphology, latticed OsteoFab PEKK scaffolds were similarly examined in in vitro and in vivo experiments.
- In 2014, an internal research study demonstrated the successful growth of bone marrow cells on 3D printed PEKK scaffolds and since then, a number of publications have examined the use of mesenchymal stem cells (autologous, adipose-derived and human synovial fluid-derived) on PEKK scaffolds in critical size defects.
- In 2016, Adamzyk et al. studied the use of PEKK scaffolds with autologous mesenchymal stem cells in a sheep calvarial defect model and found that 3Dprinted PEKK scaffolds allowed for the adherence, growth, and osteogenic differentiation of human and ovine stem cells, with considerable amounts of newly formed bone in all PEKK groups.
- In 2017, Roskies et al. similarly studied 3D-printed PEKK scaffolds with adipose-derived stem cells for the reconstruction of critical size mandibular defects. This group determined that the PEKK scaffolds presented a promising solution to improve bone-implant interfaces and biomechanical attributes of implanted materials.
This work culminated into a 2019 publication in Nature that established a definitive link between OsteoFab PEKK and bone regeneration. In vitro results of the study demonstrated the ability of human synovial fluid mesenchymal stem cells to attach, proliferate and differentiate on PEKK scaffolds, and in vivo results showed strong evidence of new bone formation. Regardless of stem cell seeding or defect model, native OsteoFab PEKK test groups have demonstrated bone apposition, bone ongrowth and improved biomechanical properties, making OsteoFab PEKK a more desirable, fully-functional implant material.
OsteoFab PEKK has also been shown to exhibit antibacterial characteristics.
- In 2017, a study published in the International Journal of Nanomedicine examined the antibacterial potential of OsteoFab PEKK given its material chemistry and rough surface. The results showed that OsteoFab PEKK provides an inherent, antibacterial environment and demonstrated decreased bacterial adhesion and growth when compared to PEEK, including a 40% to 55% higher antibacterial effect when examined using a Live/Dead assay on the native surface.
- In 2020, a follow-up study was initiated to better understand the mechanisms of this observed antibacterial property. The follow-up study showed a greater adsorption of the proteins casein, mucin and lubricin to OsteoFab PEKK when compared to PEEK and titanium surfaces. Casein, mucin and lubricin are endogenous proteins and are known to decrease bacterial attachment and growth. With the greater adsorption of these proteins, attributed to the similarity in surface energy between the proteins and PEKK, there was a clear correlation of the increased adsorption to significantly decreased bacterial colonization on OsteoFab PEKK compared to PEEK and titanium. This result was consistent across all bacteria tested, which included S. epidermidis, P. aeruginosa and MRSA. The Live/Dead assay results also illustrated fewer viable bacterial colonies on PEKK when compared to PEEK and titanium surfaces, which was consistent with the study published in 2017.
An in-depth technical summary of OsteoFab PEKK, as well as its additive manufacturing process, biocompatibility and surface technology, can be downloaded in a white paper published by OPM.
Andrus Maandi is Oxford Performance Materials, Inc. – Senior Product Development Engineer. Andrus primarily works on biomedical design and development projects with regard to R&D and regulatory submissions. This includes work on new products, supporting material, animal and cadaver studies, and filing U.S. submissions for medical device clearances. Throughout his time at OPM, Andrus has successfully applied his knowledge of additive manufacturing to help obtain medical device clearances via several regulatory pathways. Andrus joined OPM in 2014 and holds a bachelor’s degree in Biomedical Engineering from the University of Connecticut, as well as minors in Materials Science Engineering and Mathematics.