Success rate figures for total joint arthroplasty are typically based on revision rates, and do not reflect patients’ satisfaction or quality of life. Neither do they take into account the patient’s physical mobility after a surgical procedure.1 In order to reduce the need for revision, many studies have focused on identifying reasons for the failure of total hip replacements (THR). Aseptic loosening is well recognized as having a significant impact on the longevity of THRs.2 Various factors such as age, gender, body mass index, activity level3,4,5 and thickness of the cement mantle6 may predispose people to aseptic loosening. Sochart7 recommended ongoing radiological assessment of the hip following THR, so that closer follow-up can be instigated as soon as loosening or osteolysis becomes apparent on x-ray.
There is evidence to suggest that physical activity (PA) helps to maintain cortical bone after THR,8 which is important as bone loss can be a contributor to aseptic loosening.9 However, activity levels can also be thought of as a measure of the frequency and intensity of use of the prosthesis, and there is evidence to suggest that a too-high level of physical activity is a risk factor for early prosthetic failure following THR, especially in younger patients4,10 and in particular, younger men.11 Assuming that PA reflects clinical outcome, we could think of assessing success or failure of the surgical intervention by simply measuring the mobility post-operatively, comparing against pre-operative performance and prescribing patient specific activity targets. The PA data will enable the primary physicians to triage the process of optimal referral to orthopaedic surgeons or physiotherapists. The optimal time for the joint replacement surgery can be defined by constant monitoring of trends in the patient’s level of activity, avoiding costly delays and premature surgery, and thus posing a risk of multiple revisions throughout the patient’s life.
The purpose of this study was 1) to evaluate the feasibility of acquisition of mobility data of individual patients undergoing THR; 2) to provide a basis for an informed decision of what self-reporting instruments should be proposed for the large pilot study of a newly developing device for documenting PA levels in patients following THR and Total Knee Replacement (TKR); 3) to detect possible trends in the PA data sets and advise what regression trend would describe the mobility data patterns and 4) to compare self-reporting instruments used in this study with recorded PA data to evaluate potential similarities and discrepancies in order to highlight potentials for an alternative method of functional outcome monitoring using PA data.
Materials and Methods
This was a pre-pilot study in preparation for a large prospective randomized clinical trial testing a proprietary PA monitor. The pre-pilot study was designed as a case series of four patients undergoing surgical treatment THR and monitored for their level of physical activity for four to 12 weeks. Patients were selected according to the inclusion criteria, which were, 1) patients referred to an orthopaedic surgeon for THR for osteoarthritis or rheumatoid arthritis of the hip; 2) age 60 to 79 years and 3) Body Mass Index between 19.5 and 29.9. The proposed sample size for this pre-pilot study was two men and two women.
Activity levels were recorded using the activPALTM professional one axis accelerometer. (Professional Activity Logger, PAL Technologies Ltd., Glasgow, U.K.) This is a commercially available motion sensor, dimensioned 35mm x 53mm x 7mmand weighing 20 grams. The device is attached to the wearer’s thigh using a PALstickiesTM double sided hydrogel adhesive pad. The device is equipped with a piezoresistive accelerometer sensor, capable of detecting acceleration in one dimension of up to 2G with a sampling frequency of 10Hz and recording interval of 0.1s. The device records a person’s daily physical activity and can log activity for up to seven days at a time. The data is retrieved and processed using a personal computer. A custom-written software applies a proprietary algorithm to the data so that the activity can be classified into periods spent sitting, standing and walking (stepping). The system assumes that periods of sedentary activity (sitting and lying) can be classified as inactive and all upright activities as active. According to the manufacturer’s listed output characteristic, the activPAL professional accelerometer provides activity duration analysis and stepping time by cadence with resolution of 1s and steps taken with an accuracy of 99 percent with the resolution of step interval one step/minute.
Patients were asked to complete the SF36, the SF6D and the EuroQol 5D (EQ5D) questionnaires four times during the duration of the study: at enrollment (pre-admission visit), at admission to the hospital, at the time of discharge from the hospital and at the follow-up visit (about six weeks post-operatively). The SF36 is the most widely used measure of general health in clinical studies. The EQ5D is one of the measures used when utility values are required for economic evaluation, and has been recommended in the assessment of THR;12,13 the SF6D, which is based on the SF36, is an alternative measure for obtaining utility values. The disease specific questionnaires, Harris Hip score (HHS:often used clinically to assess the post-operative clinical outcome) and Western Ontario McMaster Universities Osteoarthritis Index (WOMAC Index: recommended as a patient-centred measure for patients undergoing hip replacement)12,13 were completed in this study.
After enrollment to the study, patients were asked to wear the activPAL every day from the day following enrollment until the first post-operative follow-up visit. The device was worn from the time of getting up from the bed in the morning to going to bed at night. The trends of the level of PA pre- and post-operatively were analyzed to establish the regression curves and regression equations for the pre- and post-operative period.
Results
Demographic data for each patient are presented in Exhibit 1.
Exhibit 1: Demographic and Clinical Data of Study Participants
Patient Number | Age | Gender | BMI | Orthopaedic Diagnosis | Non-Orthopaedic Diagnosis |
| 1 | 60 | Male | 25.6 | Left hip OA (for THR), Right hip post THR | None |
| 2 | 63 | Female | 25.2 | Right hip OA (for THR), Left hip post THR | None |
| 3 | 78 | Male | 29.3 | Right hip OA (for THR), Left hip OA | High blood pressure (controlled) |
| 4 | 72 | Female | 21.6 | Left hip OA (for THR), Right hip post THR | High blood pressure (controlled) |
The pre-pilot study demonstrated the feasibility of recording PA data over a prolonged period of time using physical activity monitors attached to the patients’ skin, registering steps with a frequency of 10Hz. A high volume of the data was successfully recorded, transferred and processed. None of the participants complained regarding inconvenience (including skin irritation) of wearing the activity-monitoring device adhered to the skin every day for up to 90 days.
The results from the HHS and WOMAC Hip Index were similar enough to justify usage of only one of these two instruments in further studies. Results recorded from EQ5D, SF36 and SF6D demonstrated similarities in the initial and the final scoring. This fact, and information from other published studies (EQ5D)12,13 will enable the usage of only one instrument in the upcoming studies.
Activity data for all patients was collected and entered into Microsoft Excel, and is presented in Exhibit 2.
Exhibit 2: Post-operative Physical Activity
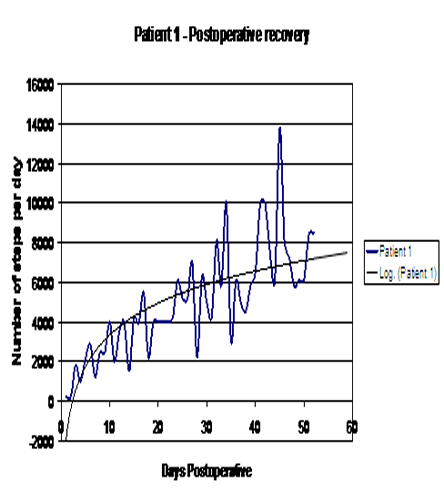

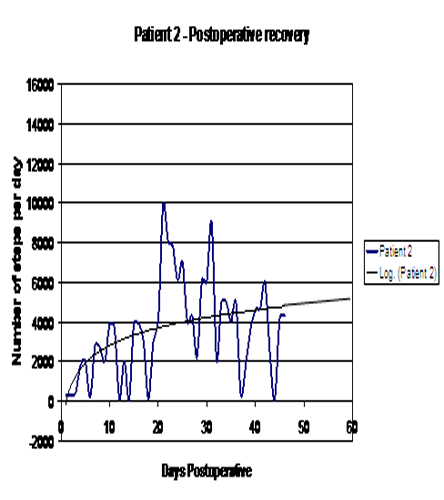

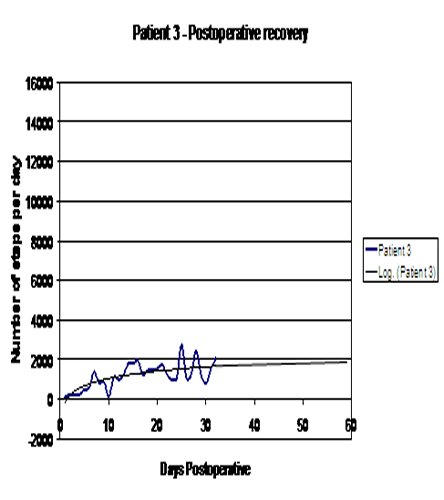

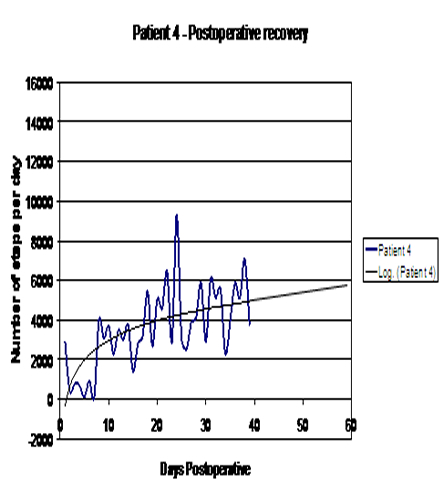

Analysis of the pre-operative data revealed that the PA before surgery declined in 3 out of 4 patients in the weeks leading to the surgery. Analysis of the data from all four participants reveals a similar pattern, with physical activity declining at varying speed in the weeks preceding surgery, following a steady increase at a similar pace after surgery. (See Exhibit 3.)
Exhibit 3: Physical Activity Performance Before and After Surgery
| Patient Number | Mean number of steps per day at pre-admission visit (entry to the study) | Mean number of steps per day at follow-up visit (exit from the study) | Difference | Percent of number of steps compared to the level of pre-admission visit |
| 1 | 4,541 | 7,285 | 2,744 | 160% |
| 2 | 3,755 | 4,733 | 978 | 126% |
| 3 | 3,940 | 1,666 | -2,274 | 42% |
| 4 | 9,263 | 5,013 | -4,250 | 54% |
This finding contrasts with the results obtained from self-reporting questionnaires in which all patients scored equally high in clinical assessment, suggesting that the clinical assessment instruments may not present a full picture of patients’ mobility behavior. On the “well-being” questionnaires, Patient 2 scored significantly lower than other participants, yet the physical activity recording demonstrates quite a satisfactory recovery after surgery, perhaps indicating additional factors playing a role in the final self assessment of the patients “well-being.” The expected excellent result of the arthroplasty at the time of the follow-up visit should result in an increased number of steps and an increased ratio of active/non-active time. (See Exhibit 4.) This pattern was only observed on Patient 2.
Exhibit 4:Summary of Results from Self-reported Questionnaires, activPAL Recording
| Self reporting instruments | Physical activity monitoring | |||||
| Patient Number | HHS + Pre-post operative | WOMAC Index + Pre-post operative | EQ5D + Pre-post operative | SF6D + Pre-post operative | No. of steps + pre-post operative | Activity Ratio + pre-post operative |
| 1 | +++ | +++ | +++ | ++ | ++ | ¯ |
| 2 | + | ++ | + | + | + | + |
| 3 | +++ | +++ | +++ | +++ | ¯ | ¯ |
| 4 | + | + | +++ | + | ¯ ¯ | ¯ |
Discussion
In 2008 to 2009 in England and Wales, there were over 65,000 and over 72,000 hospital admissions for THR and TKR, respectively. (Hospital Episode Statistics, www.hesonline.nhs.uk) The issue of optimal referral from primary physician to the orthopaedic surgeon presents significant problems.14,15,16
Although the proposed concept of monitoring patients’ PA is appealing and more objective than any other method used in current practice, it has some limitations. The method relies on patients’ compliance in wearing the motion sensor. While non-compliance in wearing can be dealt with reasonable ease through automated computer detection, the issue of cheating the system by giving a device to somebody else to wear presents a larger problem. One must assume that if such a system is to be successful, patients wish to be involved in their care. There are currently no standards specifying how to convert acceleration raw data into steps. And although each manufacturer is obliged to validate their devices, details of validation are usually not publicly available. This has an impact on the reliability of modifying patient treatment based on PA data.
Analysis of the post-operative logarithmic curves (Refer to Exhibit 2.) revealed that a component of the curves which is generally linear was achieved at seven to ten days post-operatively. This fact would support our opinion that patients were recovering their mobility at a similar pace, although at different levels. The pattern of post-operative PA was in accordance with clinical wisdom and general observations of post-operative rehabilitation progress of patients after joint replacement, indicating significant improvement in mobility followed by a plateau. To the best of our knowledge, this process has not previously been quantified or monitored. Results of this investigation demonstrate that the monitoring system could be used to obtain PA data in the early post-operative period (six to eight weeks) and several potentially diagnostic and predictive factors can then be measured. When comparing results from self-reporting questionnaires and PA recording, there was some discrepancy between the information provided by patient/surgeon and recordings from the motion sensor, especially in the cases of Patients 3 and 4. It is not quite clear why Patient 4 did not achieve the pre-operative level of activity, yet his post-operative scores were very high. Compared with other study participants, Patient 4 gained the least on clinical or “well being” scores, and did not improve dramatically when comparing the pre- and post-operative number of steps. All of the above information has led to other questions. Was Patient 4 operated at the correct time in the progression of the osteoarthritis? Was this surgery a functional success?
Additional research needs to be undertaken to understand the predictive value of certain easily and objectively measurable factors, which can be obtained by a monitoring system and used as predictors of the functional outcomes. Should those factors be identified and validated, changes to the current practice of when and upon whom to operate can be advised. Potential factors identified in this research could be the number of steps, activity ratio, pain level and pain controlled drug usage pre- and post-operatively. Indications will be provided for the most sensible time for joint replacement intervention during the natural progression of arthritis of each individual patient, offering the potential for a complete functional recovery. Moreover, the rehabilitation process can be tailored and updated based on a real-time basis to ensure that the physical activity of the individual patient stays within the prescribed limits. Long term PA post-operative monitoring may offer primary care physicians an excellent evaluation tool, reflecting the progress, pace and level of the rehabilitation process at an acceptable cost to the healthcare system.
Acknowledgments
This article was co-authored by Ian Revie, BEng, Ph.D.; Mayank Roy, MBBS, MRCS; Sameh Sidhom, MBBCh, FRCS (T&O); Michal Slomczykowski, M.D., Ph.D.
The authors wish to thank the DePuy International, a Johnson & Johnson Company, for partly sponsoring this program. Part of this publication formed the master thesis of one of the authors (M.S.) for Master Degree in Health Research Services and Technology Assessment at School of Health and Related Research University of Sheffield, U.K.
REFERENCES
1. Ulrich SD, Seyler TM, Bennett D, Delanois RE, Saleh KJ, Thongtrangan I, et al. “Total hip arthroplasties: What are the reasons for revision?” Int Orthop 32(5):597-604,2008.
2. Dayton MR and Incavo SJ. “Component loosening in total hip arthroplasty.” Semin Arthroplasty 16(2):161-170,2005.
3. Goldsmith AA, Dowson D, Wroblewski BM, Siney PD, Fleming PA, Lane JM, et al. “Comparative study of the activity of total hip arthroplasty patients and normal subjects.” J Arthroplasty 16(5):613-9,2001.
4. Munger P, Roder C, Ackerman Liebrich U and Busato A. “Patient-related risk factors leading to aseptic stem loosening in total hip arthroplasty: a case control study of 5,035 patients.” Acta Orthop 77(4):567-74,2006.
5. Schmalzried TP and Huk OL. “Patient factors and wear in total hip arthroplasty.” Clin Orthop Relat Res 418:94-97,2004.
6. Malik MH, Fisher N, Gray J, Wroblewski BM and Kay PR. “Prediction of Charnley femoral aseptic loosening by early post-operative radiological features.” Int Orthop 29(5):268-71,2005.
7. Sochart DH. “Relationship of acetabular wear to osteolysis and loosening in total hip arthroplasty.” Clin Orthop Relat Res 363:135-150,1999.
8. Rosenbaum TG, Bloebaum RD, Ashrafi S and Lester DK. “Ambulatory activities maintain cortical bone after hip arthroplasty.” Clin Orthop Relat Res 450:129-137,2006.
9. Li C, Granger C, Del Schutte H Jr, Biggers SB Jr, Kennedy JM and Latour RA Jr. “Failure analysis of composite femoral components for hip arthroplasty.” J Rehabil Res Dev 40(2):131-145,2003.
10. Sechriest VF 2nd, Kyle RF, Marek DJ, Spates JD, Saleh KJ and Kuskowski M. “Activity level in young patients with primary total hip arthroplasty: a 5-year minimum follow-up.” J Arthroplasty 22(1):39-47,2007.
11. Flugsrud GB, Nordsletten L, Espehaug B, Havelin LI and Meyer HE. “The effect of middle age body weight and physical activity on the risk of early revision hip arthroplasty. A cohort study of 1,535 individuals.” Act Orthop 78(1):99-107,2007.
12. Ostendorf M, Buskens E, van Stel H, Schrijvers A, Marting L, Dhert W, et al. “Waiting for total hip arthroplasty: avoidable loss in quality time and preventable deterioration.” J Arthroplasty 19(3):302-9,2004.
13. Ostendorf M, van Stel HF, Buskens E, Schrijvers AJ, Marting LN, Verbout AJ, et al. “Patient-reported outcome in total hip replacement. A comparison of five instruments of health status.” J Bone Joint Surg Br 86(6):801-8,2004.
14. Raymont A, Morgan S, McLeod D, Dowell A, et al. “New Zealand general practitioners’ non-urgent referrals to surgeons: who and why?” N Z Med J121(1275):57-64,2008.
15. Rosemann T, Joos S and Szecsenyi J. “The management of osteoarthritis by general practitioners in Germany: comparison of self-reported behaviour with international guidelines.”Orthopade37(1): 69-74,2008.
16. Thies-Zajonc, Szecsenyi J, Kochen M and Kohle M. “Patient initiative and referral decision of the primary care physician.” Gesundheitswesen59(10):561-565,1997.
17. Dias RC, Dias JM and Ramos LR. “Impact of an exercise and walking protocol on quality of life for elderly people with OA of the knee.” Physiother Res Int 8(3):121-130,2003.
18. Ditmyer MM, Topp R and Pifer M. “Prehabilitation in preparation for orthopaedic surgery.” Orthop Nurs 21(5):43-51,2002.
19. Friesner D, Neufelder D, Raisor J and Khayum M. “Benchmarking patient improvement in physical therapy with data envelopment analysis.” Int J Health Care Qual Assur Inc Leadersh Health Serv 18(6-7):441-57,2005.
Jon Conroy,BSc, MB ChB, MSc, FRCS (Eng), FRCS (T&O) is a fellowship trained hip and knee specialist at Harrogate District Hospital. He has a busy National Health Service practice at which the vast majority of surgery is hip or knee related. He holds a Masters degree in mechanical engineering from Leeds University. His research interest in physical activity monitoring after joint replacement has led to this study looking at this revolutionary device, which helps in deciding the appropriate time for joint replacement.
Ian Revie, BEng, Ph.D., is a shareholder and Chief Executive Officer for Activ4Life Healthcare Technologies Limited.
Mayank Roy, MBBS, MRCS, is a surgical resident in Yorkshire, U.K. He was entitled with his surgical membership degree from London.
Sameh Sidhom, MBBCh, FRCS, is a fellowship trained staff orthopaedic surgeon at Harrogate District Hospital, U.K.
Michal Slomczykowski, M.D., Ph.D., is a shareholder and director for Activ4Life Healthcare Technologies Limited.
This article also appeared in ORTHOPRENEUR®, November/December 2010.